April 21, 2026
Coping with PTSD / CPTSD
Living life differently, with Diverse Abilities.
Author

Coping with PTSD/CPTSD: Understanding & living with Post-Traumatic Stress
The information in this post is not meant to be comprehensive, only to give basic information on this disabling illness and to provide resources to seek more information or help.
Post-Traumatic Stress Disorder (PTSD) and Complex Post Traumatic Stress Disorder (CPTSD) are mental health conditions that can develop in individuals who have experienced a traumatic event or events. Traumas can encompass a wide range of experiences such as combat, natural disasters, childhood neglect, childhood or adult physical or sexual assault, accidents, or witnessing a disturbing event. Not everyone who experiences trauma develops (C)PTSD, but for those of us who do, it significantly impacts our daily life and well-being, both asleep and awake.
Symptoms of (C)PTSD can be grouped into several categories and can vary in intensity and duration from person to person as no two peoples’ experiences are the same, nor are our responses. The symptoms typically persist for months or years prior to diagnosis and can be divided into groups.

Intrusive Thoughts
Intrusive thoughts are unwelcome, involuntary thoughts, images, or unpleasant ideas that range from annoying to terrifying. They cause much distress and are difficult to impossible to manage or eliminate. Catastrophizing often accompanies intrusive thoughts.
Avoidance & Numbing
Some of us living with (C)PTSD may go to great lengths to avoid reminders of the traumatic event, including places, people, conversations, foods, or activities that trigger distressing memories. We also often avoid crowds of people, bright lights, and noise as they are overwhelming stimuli. This can lead to emotional numbness, detachment, and a loss of interest in previously enjoyed activities.

Image Description:
It reads "some disabilities look like this" with 3 people icons below (a person in a wheelchair, a person with a cane, and a person missing a leg). Then, it reads "some look like this" with what appears to be a fully able-bodied person below.

Negative Changes in Thinking & Mood
(C)PTSD can lead to persistent negative thoughts about oneself or the world, as well as distorted beliefs, guilt, and a sense of isolation. This group of symptoms may also include difficulty concentrating, memory problems, and an overall negative emotional state.
Arousal & Reactivity
Those living with (C)PTSD may become easily startled, experience heightened anxiety, irritability, have trouble sleeping, and engage in self-destructive behaviors like reckless driving, or self-medicate through substance abuse. Every person who has had or who lives with (C)PTSD, experiences it differently.
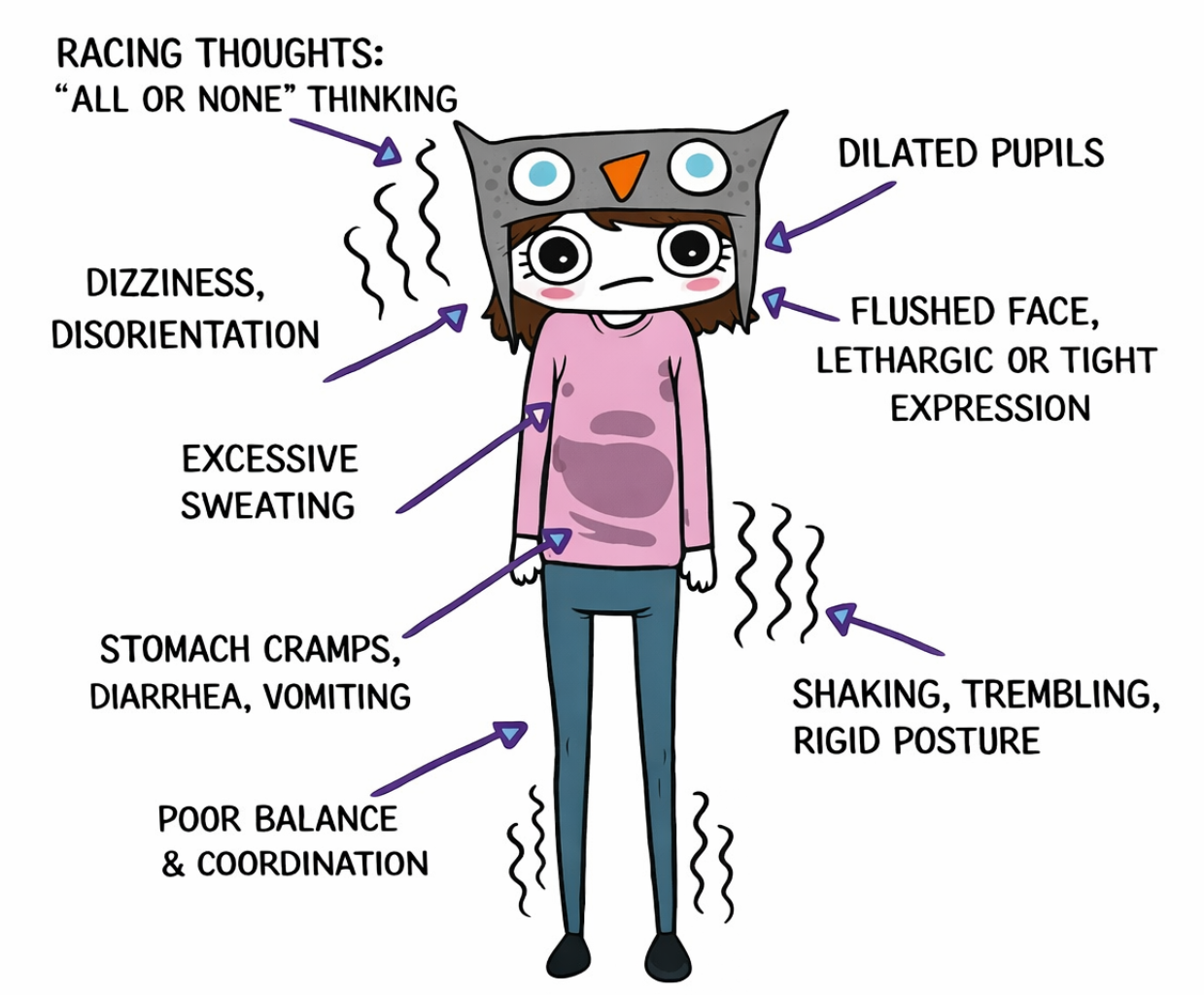
Image Description:
The image has arrows that point to the body to show how physical symptoms can present in (C)PTSD.
- Racing Thoughts: "All or None" Thinking
- Dizziness, Disorientation
- Dilated Pupils
- Flushed Face, Lethargic or Tight Expression
- Excessive Sweating
- Stomach Cramps, Diarrhea, Vomiting
- Shaking, Trembling, Rigid Posture
- Poor Balance & Coordination
Insomnia / Sleep disturbance / Nightmares
People with (C)PTSD experience varying severities of insomnia and nightmares – sleep rarely is restorative or restful for us as our symptoms don’t rest. We have vivid, terrifying, and disturbing nightmares and often lash out physically in our sleep to defend ourselves from what we are experiencing in these nightmares. Unlike people without (C)PTSD, waking up and “shaking off” these nightmares can be virtually impossible and they will continue to haunt our waking hours, often making us fearful to fall asleep again, no matter how exhausted we are.
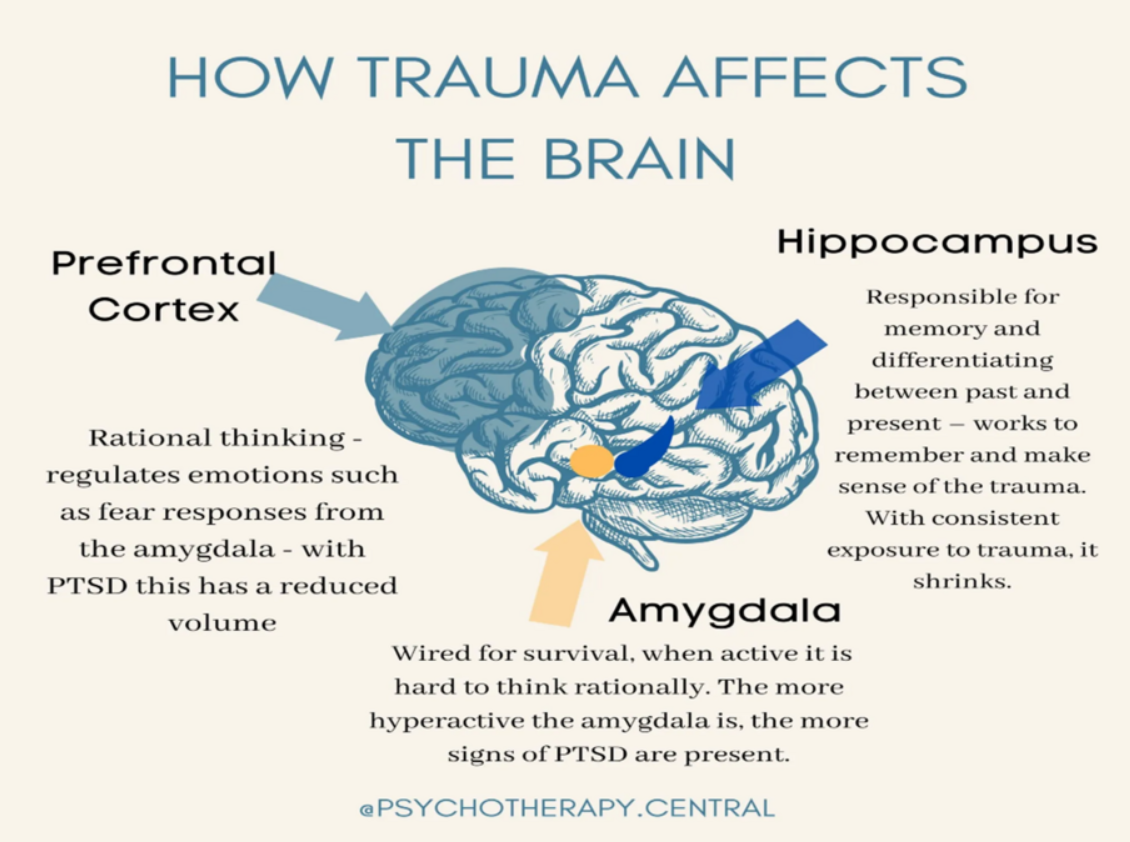
Image Description:
Title: "How Trauma Affects the Brain"
- An arrow pointing at the brain's prefrontal cortex, with an explanation stating: Rational thinking regulates emotions such as fear responses from the amygdala - with PTSD, this has a reduced volume.
- An arrow pointing to the amygdala, with an explanation stating: Wired for survival, when active, it is hard to think rationally. The more hyperactive the amygdala is, the more signs of PTSD are present.
- An arrow pointing to the hippocampus, with an explanation stating: Responsible for memory and differentiating between past and present - works to remember and make sense of trauma. With consistent exposure to trauma, it shrinks.
Image provided by "@Psychotherapy.central"
Suicidal Thoughts
Suicidal thoughts / ideation / impulses are a sad hallmark of (C)PTSD. It can seem like the only way to escape the unrelenting symptoms, the only solution. Fortunately, societal and medical knowledge of this has grown and there are crisis resources available. Links to some of these are provided at the end of this post.
Dissociation / Depersonalization / Derealization
Depersonalization is where you have the feeling of being outside yourself and observing your actions, feelings or thoughts from a distance. Derealization is where you feel the world is unreal – almost like you’re watching a movie. People and things around you may seem "lifeless" or "foggy". These things are not readily apparent to observers such as family, friends, medical providers, or the general public. Observers may think the person is being standoffish, rude, disrespectful, withdrawn, or overly quiet. The person experiencing the symptoms may feel too ashamed to verbalize what they’re experiencing for fear of rejection or shaming, and instead isolate themselves.
(C)PTSD causes physical changes to our brains, further complicating our ability to “overcome” the symptoms. For this reason, (C)PTSD is now known to be a brain injury, verified through research, and scanning of the brain by Functional Magnetic Resonance Imaging (fMRI). Scholarly articles about this can be readily found on the internet.
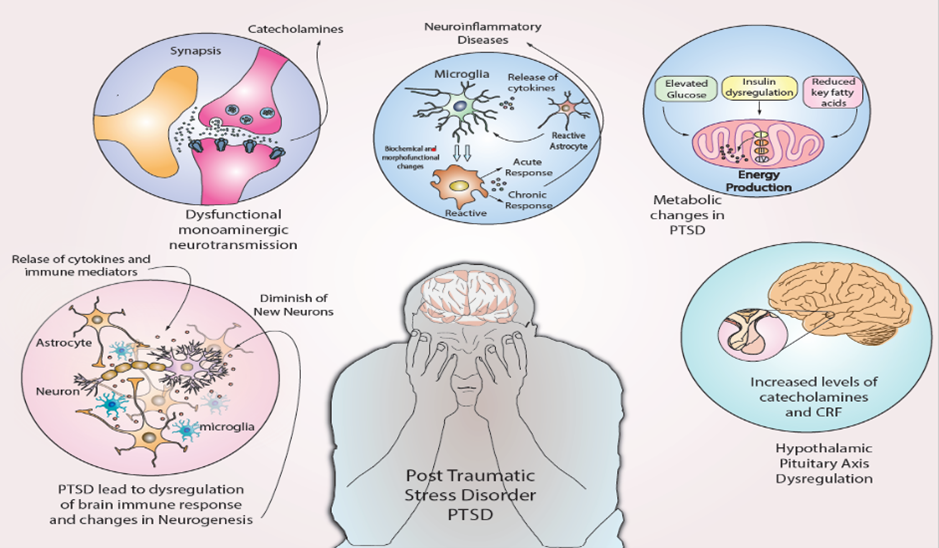
Image Description:
This is an educational infographic about Post-Traumatic Stress Disorder (PTSD) and the biological changes that can occur in the brain and body. The diagram uses soft pastel colors, including blues, pinks, and light grays, and places a distressed human figure in the center surrounded by five circular illustrations that explain different neurological and metabolic processes associated with PTSD.
At the center of the image is a gray silhouette of a person shown from the chest up. The person is holding their head in both hands, covering much of their face, suggesting emotional distress, overwhelm, or psychological suffering. A simplified drawing of a brain is visible inside the head area. Below the figure are the words: "Post Traumatic Stress Disorder (PTSD)."
Surrounding the central figure are five circular panels:
Top Left: Dysfunctional Neurotransmission
The first circle shows a close-up illustration of a synapse, the space where nerve cells communicate. Two nerve endings are colored pink and orange, with small chemical messenger particles traveling between them. The label reads "Dysfunctional monoaminergic neurotransmission." Above the illustration are the words "Synapsis" and "Catecholamines." This panel suggests that PTSD may affect the way brain cells communicate using neurotransmitters such as dopamine and norepinephrine.
Top Center: Neuroinflammatory Diseases
The second circle depicts several brain immune cells, including microglia and astrocytes. Arrows connect the cells, illustrating a chain reaction of inflammation. Labels include "Microglia," "Reactive Astrocyte," "Release of cytokines," "Acute Response," and "Chronic Response." The title above the circle is "Neuroinflammatory Diseases." This section shows how inflammation in the brain may contribute to PTSD-related changes.
Top Right: Metabolic Changes in PTSD
The third circle contains a pink mitochondrion, the cell structure responsible for producing energy. Around it are three labelled boxes: "Elevated Glucose," "Insulin Dysregulation," and "Reduced Key Fatty Acids." Beneath the mitochondrion are the words "Energy Production." The overall title is "Metabolic Changes in PTSD." This panel indicates that PTSD may affect how the body processes and produces energy.
Bottom Left: Immune Dysregulation and Reduced Neurogenesis
The fourth circle contains a network of neurons, astrocytes, and microglia shown in shades of yellow, gray, and blue. Arrows point to inflammatory activity among the cells. Labels include "Release of cytokines and immune mediators," "Astrocyte," "Neuron," "Microglia," and "Diminish of New Neurons." Text below the circle states that PTSD leads to dysregulation of the brain's immune response and changes in neurogenesis, meaning the formation of new brain cells may decrease.
Bottom Right: Hypothalamic-Pituitary Axis Dysregulation
The fifth circle contains a side-view illustration of a human brain in beige and tan tones. A magnified inset highlights a small structure near the base of the brain associated with hormone regulation. The label reads "Increased levels of catecholamines and CRF." Beneath the circle is the title "Hypothalamic Pituitary Axis Dysregulation." This section suggests PTSD can alter the body's stress-response system and hormone regulation.
Image Description:
Title: "PTSD & The Brain: Why People Can't Just 'Snap Out Of It'"
Top Left Box: Prefrontal Cortex
A pink rectangular box labelled "Prefrontal Cortex" describes the role of this brain region.
Under a blue checkmark labelled "Normal", the text states:
- Complex thinking
- Decision making
- Appropriate behavior
Under an orange X labelled "PTSD", the text explains:
- Dysfunctional thought processes and decision making
- Inappropriate responses to situations
This section indicates that PTSD can impair reasoning, judgment, and the ability to respond appropriately to everyday circumstances.
Top Right Box: Amygdala
A second pink box labelled "Amygdala" explains the brain's fear and threat detection center.
Under a blue checkmark labelled "Normal", the text states:
- Sets off fight-or-flight in response to danger
Under an orange X labelled "PTSD", the text explains:
- Sets off fight-or-flight in response to memories or thoughts about danger
This section highlights how PTSD can cause the brain to react as though danger is present even when the threat exists only in memories, reminders, or intrusive thoughts.
Bottom Left Box: Hypothalamus (HPA) Axis
A third pink box is labelled "Hypothalamus (HPA) Axis."
Under a blue checkmark labelled "Normal", the text states:
- Releases hormones like cortisol to help manage and direct responses to stressors
Under an orange X labelled "PTSD", the text explains:
- Becomes overactive, leading to imbalances in hormone levels
- Increases stress and anxiety
This section describes how PTSD can disrupt the body's stress-response system, contributing to ongoing anxiety and heightened stress reactions.
Bottom Right Box: Memory Processing Region
A fourth pink box describes the brain area responsible for memory formation and retrieval, likely referring to the hippocampus, although the structure is not specifically named in the graphic.
Under a blue checkmark labelled "Normal", the text states:
- Transfers and stores information into memories
Under an orange X labelled "PTSD", the text explains:
- Stores memories incorrectly
- Affects memory retrieval
This section suggests that PTSD can alter how traumatic experiences are stored and recalled, contributing to flashbacks, intrusive memories, and difficulty distinguishing past events from present reality.
Image provided by "@RealDepressionProject"
Coping strategies for some of us living with (C)PTSD:
- Seek Professional Help
- If you or someone you know is experiencing symptoms of (C)PTSD, it is essential to reach out to a mental health professional who is trauma informed. Trauma counseling is a specialty field and not every counselor, therapist, or psychologist has this specialized education.
- Psychotherapeutic treatment options are evolving and may include talk therapy, Cognitive Behavioral Therapy (CBT), Cognitive Processing Therapy (CPT), Eye Movement Desensitization and Reprocessing (EMDR), Dialectical Behaviour Therapy (DBT), and in some cases, medication.
- Social Support could be spending time with friends and family for emotional support. Sharing your feelings and experiences with people you trust might help alleviate the isolation that often accompanies (C)PTSD.
- Prioritize self-care activities. Regular exercise (getting up and moving) doesn’t mean you have to run a marathon. Being mindful of eating healthy food choices can make a difference in mood and energy. Making sure you get adequate sleep - easier said than done as sleep disturbance and insomnia are key features of (C)PTSD - to help manage some of the symptoms. These can have a positive impact on your overall well-being.
- Practice relaxation and stress-reduction techniques like deep breathing, meditation, yoga, or progressive muscle relaxation to help manage anxiety and arousal symptoms.
- Avoid using alcohol, caffeine, or drugs to cope with (C)PTSD as they can lead to further problems. It's important to seek healthier coping methods.
- Maintaining a regular daily routine can provide structure and predictability for some, which can help reduce anxiety and provide a sense of stability.
- Educate yourself so you have a better understanding of (C)PTSD and its symptoms. Knowledge can be empowering. Knowing what to expect and how to manage it can make the condition feel less overwhelming.
- Joining support groups for those of us living with (C)PTSD can offer a sense of community and understanding. Connecting with others who have experienced similar trauma can be comforting and helpful. This can be accomplished online if you aren’t comfortable being in a group setting or if a group setting isn’t available to you.
It's essential to remember that recovery from (C)PTSD is a journey and it is different for all of us. It takes time to heal and sometimes we never completely recover, but we learn to better manage the symptoms.
It can be extremely difficult for some of us to talk about how we are feeling or if we are coping or not. If someone shares with you that they have (C)PTSD, believe them. Most people do not go around pretending to have mental health disorders if they do not. Take it as a compliment that we trusted you by sharing.
Different strategies work for different people, so it's crucial to find what works best for you with the guidance of a mental health professional. If you or someone you know is struggling with (C)PTSD, don't hesitate to seek help.
Canadian Support Resources:
- If you or someone you know is in immediate danger or need urgent medical support, call 9-1-1.
Canada Mental Health Support Website
- Click Here
- Provides detailed information that Canadians looking for mental health support services by province and territories.
Suicide Crisis Helpline
- Call or Text: 9-8-8
- Help is available 24 hours a day, 7 days a week.
Health Link Services
- Dial: 8-1-1
- This number only works in some provinces, and in some cases must be called from a landline.
- It's a free, 24/7 confidential provincial health line available across Canada to connect residents with registered nurses for non-emergency medical advice, mental health support, and dietetic services. It helps navigate care and provides symptom assessment, acting as a bridge between self-care and emergency services.
USA (United States) Support Resources:
- If you or someone you know is in immediate danger or need urgent medical support, call 9-1-1.
Suicide Crisis Hotline
- Call or Text: 9-8-8
- Visit the 988 Lifeline website: Click Here
(C)PTSD Learning Resources:
(Click the links below to explore the resources)
Book Recommendation:
Website Resources:
A Guide To Supporting Those of Us Living With (C)PTSD:
Being a support to someone living with Post-Traumatic Stress Disorder (PTSD) or Complex Post Traumatic Stress Disorder (CPTSD) can make a significant difference in our recovery and overall well-being. Here are some ways you can provide support to us who are living with (C)PTSD:
- Learn about (C)PTSD, its symptoms, and treatment options. Understanding the condition will help you empathize with us, be less confused or upset by our behaviours, and you will be able to offer more effective support.
- We really do appreciate your patience and understanding, even if we don’t always verbalize it. (C)PTSD is be a long and challenging journey. Be patient, non-judgmental, and empathetic. Avoid pushing us to talk about our trauma if we are not ready and consider that you may not be ready to hear about it, despite your best intentions. Someone with (C)PTSD will be reliving the experience you are asking them to tell you about. To their brain and body, it is not just a memory.
- If someone with (C)PTSD wants to talk, be a good listener. Let us share our thoughts and feelings at our own pace. Avoid offering unsolicited advice or solutions. The trauma(s) that caused (C)PTSD were harsh, ugly, and brutal events for us to experience and will not be easy for anyone to hear.
- Help us to feel safe and supported. This may involve creating a calm and predictable environment, avoiding triggers, and the verbal reassurance “You are safe here and now.”
- Encourage us to seek professional treatment if we have not or are not currently. Offering to help us find a suitable trauma informed therapist or psychiatrist if needed can be extremely helpful as at times when we are not motivated or in the right space, that can be an impossible task.
- If you are comfortable, you could offer to accompany us to therapy or medical appointments. This can provide emotional support and make the process less daunting for us.
- Most of us have triggers. These can be specific situations, places, or sounds that remind us of the traumatic event(s). Being mindful of these triggers and try to minimize exposure when possible.
- Respect our boundaries and personal space. Don't pressure us to participate in activities or social events if we are not ready.
- Offer us practical support such as helping with tasks like cooking, cleaning, or running errands when needed. Practical assistance can alleviate stress and allow us to focus on our recovery.
- Be aware of signs of crisis or suicidal thoughts. If you believe we are in immediate danger, seek professional help or contact a crisis hotline.
- Something you could do that could be really helpful for some of us is to find local or online support groups for individuals with (C)PTSD, that we can join. Sharing experiences with others who understand can be incredibly beneficial.
- Check in on us and our well-being but respect our need for space if we don't want to talk. Simply knowing that someone cares can be comforting.
- Please be flexible and prepared for our needs to change. What is helpful today may not be the same in the future, so be flexible in your support.
Remember that supporting those of us with (C)PTSD can be emotionally challenging, so it's essential to take care of your own well-being. Encourage us to build a support network, including mental health professionals, friends, and family members. By offering your understanding and support, you can play a crucial role in our healing process.












